(c) 1995, Willis Lamm, TrailBlazer Magazine
" FRACTURES AND SPLINTING"
By Willis Lamm
Reprinted with permission of TrailBlazer Magazine for
non-commercial use.
There are 206 bones in the human body, and every fall brings with it the possibility of breaking one.
While most of the
time we dust ourselves off and climb back on with little more than bruised muscles and bruised egos, there
are a few
instances where fractures do occur, which can prove to be serious emergencies. Whether in the barn or out
on the trail, it
is important to understand the physiology of fractures and take the correct steps early on after the
accident.
What happens during a fracture:
When a fracture occurs, a portion of a bone may chip or crack away or the bone may be completely broken.
In any event,
the bone fragments will damage nearby tissues and blood vessels, causing swelling and blood clots in the
area of the
fracture. Nearby tissue cells which lose their blood supply will die.
Undamaged tissue cells nearby the fracture site will respond to the injury by rapidly dividing in an
attempt to form a
collar of tissue surrounding the fracture site. New bone is generated from this mass of tissue in order to
eventually heal
the damaged bone.
If the fracture site is mishandled early after the injury, more soft tissues could be damaged which could
significantly
prolong healing. If the bone ends are disturbed, the disruption to the normal healing process could result
in a permanent
disability.
More critically, arteries and nerves run parallel to bones in the arms and legs. A mishandled severe
fracture could
result in a bone end severing an artery or major nerve creating a potentially fatal bleed or paralysis.
Even small
fractures, such as in a finger, can lead to a frustrating disability if not treated correctly.
Accordingly, all fractures (or suspected fractures), no matter how minor, should be taken seriously.
As there is not enough column space to discuss all of the possible fractures, here are some common
situations and basic
care concepts. Remember that each situation is different, so utilize common sense when caring for any
fracture until
professional help can be obtained.
There are two classifications of fractures, closed fractures and open fractures. Closed fractures
include any fracture
where the bone does not penetrate the skin (the skin stays closed). In such instances, proper treatment
includes
immobilizing the fracture and seeking medical help. Open fractures occur when a bone or bone fragment
breaks through the
skin or the skin and bone are broken in a traumatic, crushing injury. Proper treatment for open fractures
must also include
concern for possible infection.
�Recognizing Fractures:
An open fracture will typically be self evident due to the exposed bone. The following clues suggest you
are dealing with
a probable closed fracture:
The patient felt a bone break or heard a "snap".
The patient feels a grating sensation when he/she moves a limb. (This condition is known as
crepitus.)
One limb appears to be a different length, shape or size than the other, or is improperly
angulated.
Reddening of the skin around a fracture may appear shortly after the fall.
The patient may not be able to move a limb or part of a limb (e.g., the arm, but not the
fingers), or to do so
produces intense pain.
Loss of a pulse at the end of the extremity.
Loss of sensation at the end of the extremity.
Numbness or tingling sensations.
Involuntary muscle spasms.
Other unusual pain, such as intense pain in the rib cage when a patient takes a deep breath or
coughs.
If you discover any of these symptoms and cannot attribute them to any other obvious cause, assume them
to be symptomatic
of a fracture.
�Initial Care for Fractures:
In treating fractures, an unhurried and careful approach is best. Few fractures are life threatening
unless mishandled.
Check the patient for any more serious injuries. Make sure someone is going for help, or call 9-1-1.
Ensure your patient is
breathing and that excessive bleeding is controlled and that all open wounds are protected as best you can
from
contamination. After these elements are satisfied you can deal with stabilization of the fracture.
If you can, carefully cut away all clothing near the fracture site. You need to make sure the fracture
hasn't broken the
skin and you may be able to use the cut away material to aid in splinting. If you find an open fracture,
protect the wound
from contamination as you would any other.
No matter how soon you expect to get medical help, you should immobilize all fractures to prevent
additional injuries due
to accidental movement or muscle spasms. Immobilization can be achieved many ways; the key points being not
to worsen the
situation while immobilizing and making sure to also immobilize the joints above and below any limb
fracture.
In general, don't try to reposition fractured limbs. Unless you know what you are doing, you could sever
an artery or
nerve. If out on the trail with help a long way off, practicality may necessitate slight repositioning in
order to
accommodate make-do splinting. In such situations if a limb has no pulse or is turning purple,
repositioning may relieve
some unnatural pressure which is pinching off an artery, however the rescuer must consider that a mishandled
attempt could
result in a jagged bone end severing the compressed artery, making a bad situation much worse!
To put this tricky situation in perspective, Brady's Emergency Care, 6th Edition states:
"Angulations make
splinting and transport more difficult. They can pinch or cut through blood vessels and are painful for the
patient. They
must, however, be repositioned so they can be splinted. Not to splint would be more dangerous."
DO NOT try to straighten angulations of the wrist, ankle or shoulder or attempt to straighten any
dislocated
joint!
When splinting using sticks or other "found" objects, try make padding between the injured limb and
splint using a jacket,
shirt filled with grass, anything which can be reasonably secured and can help fill in the gaps between the
limb and the
splint material. Don't get carried away with this concept, but if you can handily make something up without
delaying the
splinting process, it will be more comfortable to the patient.
Long bone fractures in the legs and arms can benefit from mild traction when splinting. For arm
fractures where you have
help during splinting, one person can grasp the arm above and below the fracture site and apply a smooth,
steady pull until
your helper can apply the splint. If you encounter a firm resistance, crepitus or the patient experiences a
significant
increase in pain, do not attempt traction. Do the best you can to splint in the position found. Once you
successfully apply
traction, do not release it until the splint is securely supporting the limb, otherwise the retracting bone
end will cause
additional tissue damage and possibly injure a nerve or artery.
A fractured forearm should be splinted from the hand through the elbow and can be secured across the
chest with a sling if
more comfortable for the patient. Upper arm fractures should be immobilized from shoulder through the elbow
and can be
secured against the body.
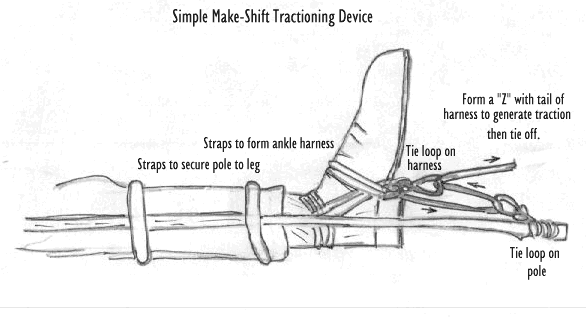
Traction for leg injuries is more difficult, and the risk of injury resulting from a failed traction
attempt is even
greater. Do not attempt leg traction until your helper is ready to apply a splint. Legs should be secured
to splints using
several ties from the ankle to the pelvis, but not directly over the fracture. If a long smooth board is
available (e.g., a
fence board), it can be secured all the way up to the armpit to improve stability.
Hip Fractures:
Hip fractures can be very serious since they actually involve the upper portion of the femur, the large
bone of the upper
leg. Hip fractures are more common in older persons, and any elderly riders who sustain a fall and complain
of hip pain
should be suspect for this injury.
Symptoms of hip fractures include sensitivity when pressure is exerted on the prominence of the hip,
swelling with or
without discoloration of the surrounding tissues, the patient is unable to move
his/her leg when on his/her back, the
suspect limb appears shorter or is rotated (usually outward).
Patients with suspected hip fractures should only be moved on a stretcher. The injured limb can be
secured to the
uninjured limb to provide splinting. If medical help is a long way off and someone can spell you if you
tire, you may find
that manual traction provides significant relief for your patient.
Fractured Hands and Ankles:
These extremities should be splinted in "positions of mechanical function", that is in as natural of a
position as
possible. The natural position of a hand is as if one were gently grasping a softball. A roll of clothing
or other padded
material can become the "ball" which can be placed in the palm before the hand is wrapped. Hands, ankles
and wrists should
be secured in whatever manner is necessary to protect them from being bumped or moving about while the
patient is being
rescued.
Fractured Ribs:
The primary concern of a suspected rib fracture is to prevent a loose piece of rib from puncturing a
lung. The best
course of action here is to keep the patient from moving around, pad and gently wrap the chest, and apply a
sling and swathe
to secure the arm on the injured side so it lays comfortably across the chest. Padding and wrapping the
chest on the trail
may be awkward, and it is not worth unnecessarily moving the patient around to accomplish this task. In
such instances
simply make the patient comfortable and discourage unnecessary movement.
Skull and Facial Fractures:
Fractures to the face and skull are serious emergencies, obviously involving the brain in the case of
skull fractures, but
also compromising the airway and breathing ability in the case of facial fractures. If you find evidence of
skull or facial
fractures you should presume the possibility of cervical spine injury also.
Decreased consciousness, deep lacerations or severe bruising, deformity, fluid from the ears, unequal
pupils, "raccoon's
eyes", and a sunken eye are all symptoms of possible skull or facial injury. If you find any of these signs
you should
presume the possibility of cervical spine injury also.
Care for skull and facial fractures includes maintaining an open airway, immobilizing the neck and spine,
and treating
wounds. Do not apply pressure, however, to any suspected fracture site! Note the patient's change in level
of consciousness
prior to the arrival of medical help as these observations may assist in the diagnosis of the extent of the
injury.
Recap of Actions:
Get assistance from competent bystanders.
Check patient; ensure airway, breathing and circulation.
Have someone go for help or call 9-1-1.
Protect possible spinal injuries.
Treat life threatening conditions.
Protect open wounds, including open fractures.
Splint fractured limbs and/or extremities, in natural or functional position, if feasible.
Avoid unnecessary movement of fractured extremities.
Apply mild traction if practical and it relieves pain while splinting is taking place.
Keep patient quiet and treat for shock.
If you have to move a patient for his/her survival, be careful and methodical, support splinted
injuries to
prevent further movement, bumping, etc., and don't move the patient any further than necessary without
proper
professional equipment.
Our thanks to TrailBlazer Magazine for permission to post this series on our web page.
You can visit the TrailBlazer website at www.horsetrails.com.
Email the author
Return to Safety Main Page
|